‘Why haven’t we heard about phages before?’ asked Evan Davis brightly on the ‘PM’ programme on May 2. He was referring to the ‘new’ miracle cure which had just been unveiled at Great Ormond Street hospital. But new it isn’t. The BBC news machine works inside a small loop, and its memory is short. Twenty years ago I published a feature in the Independent on Sunday which outlined the long history of this remarkable alternative to antibiotic medicine, and pointed to its huge future potential. For those who missed it, here is a link, and here is the article again, needing no substantial updating because the world of medicine still hasn’t woken up:
Revealed: our best hope to beat the killer ‘superbugs’
Scientists at a neglected lab in the former Soviet Union are leading the fight against a medical nightmare, writes Michael Church
· Sunday 12 September 1999 00:02
AS BRITISH hospitals face an invasion of antibiotic-resistant “superbugs”, the country’s biggest scientific conference will be urged this week to pour research effort into a cure virtually unknown outside the former Soviet Union.
Dr Paul Barrow, one of the few British experts on phage therapy – microscopic viruses extracted from sewage, which can cure some of our most deadly diseases – will tell the British Association for the Advancement of Science that phages can solve many of the problems antibiotics have caused. The viruses attack the bacteria responsible for the diseases, and while the bacteria can evolve resistance to antibiotics, they cannot do so to phages: the viruses simply evolve along with them.
For the past half-century, almost the only research into phages has been done in a decrepit building in the war-torn capital of an impoverished former Soviet republic. Working conditions are primitive at the Bacteriophage Institute in the Georgian capital, Tbilisi. Nino Chanishvili’s laboratory is a tiny attic which she shares with four other scientists. It’s swelteringly hot, the floor tiles are loose, and the sink is an ancient bedroom washbasin, yet she insists: “We may be low-tech, but we are still doing sophisticated science.”
Antibiotics once seemed the all-purpose answer to bacterial infections, but no more. Overuse has made bacteria increasingly resistant, and attention is turning once more to the studies of the Georgian researchers.
Dr James Soothill, a microbiologist at Manchester University who uses phages on burns, says a crisis is imminent. “It’s always been possible to die from a surgical infection, but within 10 years many such infections may not be treatable by antibiotics,” he said.
“When you’re developing new treatments, you have to plan years ahead, because it takes years to get from research prototype to the marketable product. Phage therapy isn’t the only alternative to antibiotics, but it has great promise.”
Phages have unique advantages over antibiotics, according to Dr Soothill. “They replicate at the place in the body where you want them. They don’t simultaneously kill most of the body’s normal, helpful bacteria. And they can multiply from one to tens of billions in a mere five hours.”
Phages can cure dysentery, septicaemias and some forms of meningitis, and have also been effective against epidemic cholera. “They are least effective,” said Dr Barrow, a microbiologist at the Institute for Animal Health, “with diseases like tuberculosis, whose bacteria multiply inside the patient’s cells.” He stressed the importance of rigour in their evaluation, saying: “If the research is not done properly, the cause of phage medicine will be set back for another few decades, as it was after some ludicrously bad field studies in the Twenties. Those led to it being completely discredited in the West.”
The Georgian institute’s work couldn’t be more topical. One of the infections its scientists are working on is staphylococcus aureus – the antibiotic- resistant bug now causing panic in the US. In the 1980s they developed an effective intravenous treatment for a less resistant form of this infection, and Dr Chanishvili’s work is a continuation of that process.
She picks up a dish whose cloudy surface is dotted with clear spots. “Each spot is where one of our viruses has destroyed the bacteria of a new pathogen which affects people with suppressed immune systems. Don’t touch!” But I have touched. “Now wash your hands. Twice!” I notice they are not wearing gloves – in Tbilisi such things are too precious for daily use.
The word bacteriophage, meaning “bacteria-eater”, was coined in the 1920s by French-Canadian microbiologist Felix d’Herrelle who – while investigating an outbreak of dysentery in Paris – discovered that a surprising variety of infections could be cured with the aid of viruses extracted from raw sewage.
One-fortieth the size of bacteria, these viruses are found wherever bacteria thrive – in oceans, in our bodies, and above all in sewage. They look like extra-terrestrials, with large heads, narrow tails, and spidery legs; they inject their prey with their offspring, which multiply so fast that the host literally bursts.
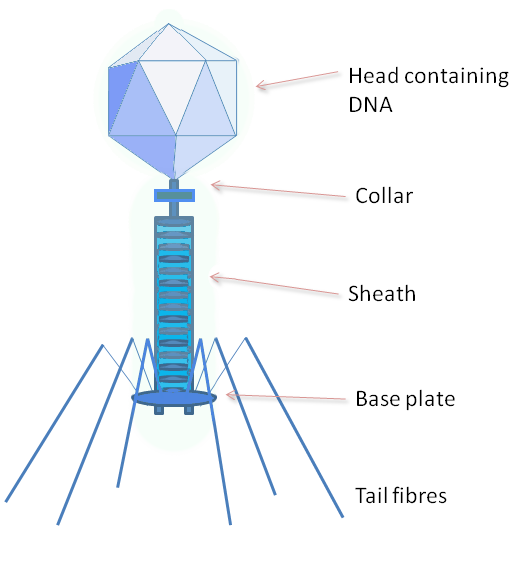 A diagrammatic representation of a bacteriophage source: Wikimedia Commons
A diagrammatic representation of a bacteriophage source: Wikimedia Commons
The beauty of phages is that, unlike antibiotics, they mutate to keep pace with the bacteria they are programmed to destroy. Their limitation lies in the fact that each can act on only one specific host. No wonder they were upstaged in the West by antibiotics, which kill everything in their path.
But they weren’t upstaged in the East. In 1923 the Georgian scientist George Eliava founded an institute in Tbilisi devoted to the ideas of D’Herrelle, an ardent Communist who settled in the Soviet Union at Stalin’s invitation. Until the demise of Communism wiped out its market, and Georgia’s civil war destroyed the local infrastructure, the institute researched new remedies and exported them to every corner of the Soviet empire. They were generally used as alternatives to antibiotics – as they still are in Tbilisi – but they were also often used in tandem.
With Georgia’s economy in ruins, Dr Chanishvili and her woefully underpaid colleagues now face huge obstacles in their attempt to join the scientific mainstream. Two years ago they almost struck a deal with an American entrepreneur which might have lifted them out of their crippling poverty. She attributes the failure of that deal to a clash of cultures, saying: “We and the Americans still carried the Cold War in our heads. There was a wall between us, mistrust on both sides.”
Her uncle, Teimuraz Chanishvili, the institute’s director, shows off the “library” he and his staff have collected, where each phage is kept in a sealed bottle at a controlled temperature – at least in theory: in practice much of their collection was wiped out during Georgia’s civil war by power cuts.
Thanks to contacts made through a BBC documentary, Dr Chanishvili has embarked on joint projects with British phage researchers investigating the campylobacter bug (food-borne, from poultry to humans), and the drug- resistant pseudomonas infection, which colonises the wounds caused by burns.
Dr Barrow is one of her collaborators. He thinks phages could offer the biggest medical breakthrough for decades. “But money would have to be committed to it. The institute next door to us has just put millions into a new vaccine research centre, but virtually nothing is being done to support research into phages. It’s a crazy situation.”
Really interesting Michael.
Richard Roques
I have just found the page but if anybody is intersted in Pharge the the following link is to a BBC Horizon programme made in 1997. https://archive.org/details/BBCHorizonS1997e13TheVirusThatCures.
We have been talking about pharge for a long long time.
Enjoy